Reverse Total Shoulder Replacement
Total shoulder replacement (TSR) describes a surgical procedure where a prosthesis or implant replaces the gleno-humeral joint (the shoulder joint).
Reverse shoulder replacement (RTSR), also known as reverse shoulder arthroplasty (RSA) has become a pivotal surgical option for patients suffering from severe shoulder dysfunction, particularly those with rotator cuff arthropathy or irreparable rotator cuff tears. This innovative procedure has evolved over the years, offering improved outcomes and expanding indications.
Reverse shoulder replacement reconfigures the shoulder’s anatomy to use the deltoid muscle for arm movement instead of the rotator cuff. This is achieved by placing a ball component on the shoulder blade (glenoid) and a socket component on the upper arm bone (humerus), effectively reversing the natural ball-and-socket joint.
Adelaide orthopaedic surgeon Dr Sunil Reddy specialises in shoulder surgery and performs TSR and reverse TSR. He routinely offers ‘patient-specific technology’ in shoulder arthroplasty – a CTscan -based 3D-prototyping technology that allows accurate placement of the glenoid (shoulder socket) component and contributes to accuracy and precision during surgery and better outcomes.
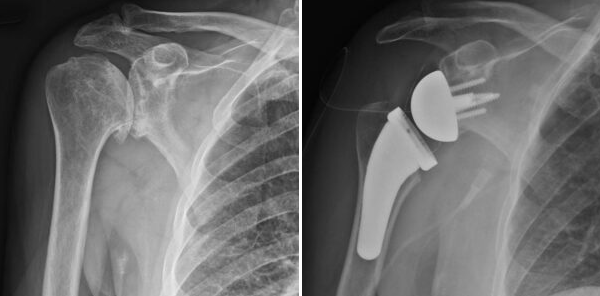
X-rays showing advanced arthritis of shoulder and postoperative picture after a reverse shoulder replacement.

3D CT reconstruction of a severely comminuted proximal humerus fracture and x-ray after reverse shoulder replacement and tuberosity reconstruction.

Another example of proximal humerus fracture treated with reverse shoulder replacement. Healed tuberosity reconstruction resulted in excellent function after six months.
Common Indications for Reverse shoulder replacement:
- Rotator cuff tear arthropathy
- Irreparable rotator cuff tears
- Severe shoulder arthritis with rotator cuff deficiency
- Severe shoulder arthritis with bone erosion and defects
- Complex fractures of the proximal humerus
- Failed previous shoulder surgeries
Fractures of proximal humerus
Where a fracture is severe, it may be very difficult to put the segments of bone back together. Blood supply to parts of the bone may also be compromised and Dr Reddy may recommend shoulder replacement in the form of a Reverse Total Shoulder Replacement ( RTSR also called RSA or Reverse Shoulder Arthroplasty). It has been proven that especially in the elderly, complex fractures of the upper humerus are most effectively treated with RTSR. This enables early mobilisation and faster recovery along with predictable restoration in function and strength.
Patient-specific technology in joint replacement
This is a CT scan-based 3D-prototyping technology where 3D models of the arthritic joint as well as jigs specific to the patient’s anatomy are manufactured. These are then used during surgery to make accurate bone cuts or bone reaming and implant the prosthesis.
Outcomes and Patient Satisfaction with Reverse shoulder replacement
Reverse shoulder replacement has shown excellent outcomes, with most patients experiencing significant pain relief and improved shoulder function. The success of the surgery largely depends on accurate diagnosis, appropriate patient selection, and meticulous surgical technique.
Please contact Dr Reddy on 08 8232 8899 to discuss your shoulder problem. He will formulate a personalised treatment plan after a thorough assessment and discussion of options, both non-surgical and surgical to achieve the best possible outcome for yourself.
Surgery
Surgery involves replacement of the ball (head of the humerus) and the socket the ball fits into.
The procedure itself, which is performed through a delto-pectoral approach, normally takes around 60-80 minutes, requires a general anaesthetic, and a hospital stay of two to three days.
Risks and complications
Dr Reddy will explain the benefits, risks, and complications of a shoulder replacement in the clinic to help you make an informed decision regarding your surgery.
Possible complications of this surgery include:
- Injury to blood vessels or nerves.
- Haematoma formation.
- The prosthesis coming loose or dislocating.
- A ‘frozen shoulder’, where the shoulder is sore and stiff.
Postoperative recovery and rehabilitation
Dr Reddy as well as the physiotherapist will see you on day one following surgery and will demonstrate exercises to be performed as well as advise on things to do and not do.
It’s important you follow the advice and rehabilitation guidelines to give yourself the best chance of recovery and an optimal outcome.
- You would likely have a regional / nerve block for pain management apart from a general anaesthetic.
- You would usually stay in the hospital for two to three days, but may stay longer depending on the recovery.
- Please take regular pain medication as advised.
- Apply ice packs five times a day for 15-20 minutes each time for the first two weeks.
- You will need to wear a sling full time for four weeks, but you can remove it thrice daily for 15-20 minutes each time to perform exercises.
- Please remove the sling for a shower, resting your arm by the side. The dressings are waterproof.
- After four weeks, you can come out of the sling to perform gentle activities of daily living.
- After six weeks, you can progress with exercises as advised by your therapist.
- Strengthening exercises usually start only after three months following surgery.
- Avoid lifting weights and push-pull movements for three months following surgery. The goal is to gradually achieve normal range of movement and strength of the shoulder over a three-to-six-month period.
- Driving is permitted only once you come out of the sling and have achieved good control of the arm and a pain-free status. This is usually by the six-to-eight-week postoperative period.
- Please follow your therapist’s advice regarding exercises and follow the rehabilitation guidelines that you can view / download below.
