Revision Total Hip Replacement
Revision total hip replacement is surgery to correct problems relating to an earlier total hip replacement (THR) procedure.
Revision hip replacement surgery is a complex and challenging procedure in the field of orthopaedics. However, recent advancements in surgical techniques, materials, and postoperative care have significantly improved the outcomes for patients undergoing this procedure. Enhanced preoperative planning, innovative implant designs, minimally invasive approaches, and better postoperative management have all contributed to increased success rates and improved patient satisfaction.
Dr Sunil Reddy is an experienced primary and revision joint replacement surgeon. To achieve the best possible outcome for problems with your existing hip replacement implant, please contact Dr Reddy on 08 8232 8899. He will discuss the nature and severity of the problem, organise advanced imaging for precise assessment of bone loss and aid pre-operative planning and formulate a plan that best suits your needs.
The Australian National Joint Replacement Registry lists the following as important reasons for revision of a THR.
- Loosening of artificial hip components– where the artificial joint has been in place for a long time or has been subject to considerable wear and tear, the components may become loose. Loosening is often a result of osteolysis.
- Osteolysis– this is where the bone deteriorates due to an immune response to small fragments of the plastic components which break off as part of normal wear and tear. The immune response attacks healthy sections of bone as well as the particles released, which can lead to instability in the artificial hip joint.
- Repeated dislocation of artificial joint.
- A fracture near the site of the artificial joint– called a periprosthetic fracture, this is often caused by a fall or other accident.
- Infection– where infection occurs within the artificial joint, the infection must be treated and existing components will need to be replaced.
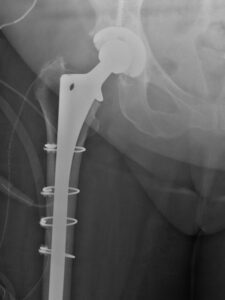
Revision hip surgery often involves osteotomy to extract the previous component and longer stems with distal fixation or fixation along the entire length of the stem.
Procedure
A revision total hip replacement is generally more complex than the first operation and is often associated with more bleeding and higher risk of complications than primary THR.
When revision is performed for infection it could be a two-stage procedure: the first stage to remove the infected components and place an antibiotic-loaded spacer, and the second stage to replace the spacer with a definitive new hip replacement.
After an incision is made, a normal revision surgery is a three-step process:
Stage 1 – removal of existing artificial hip components
It’s important these components are removed with minimal damage to the remaining bone and surrounding tissue. If cement has been used to fix the components to the bone then this must be removed, often with the aid of an ultrasonic machine that dissolves the existing cement.
Stage 2 – bone graft/attachment of artificial bone augments
If any bone has been lost this must be replaced either with a bone graft, generally using a section of the patient’s own bone harvested from another bone in the body, or donor bone from a ‘bone bank’ or prosthesis with built-in metal supports.
Stage 3 – fixing of the new artificial hip joint components
As with the normal total hip replacement procedure, this may involve using cement to fix the components in the hip socket and thigh bone. Revision implants usually are longer than those used in primary THR and may involve more constraint at the bearing surface.
Postoperative recovery and rehabilitation
Please see the section on total hip replacement for an overview of ‘things you need to know’ following a THR. Recovery and rehabilitation following a revision surgery is along the same lines, but may be more prolonged considering the complex nature of surgery. Revision hip replacements also tend to have increased complication rates compared to primary THR and this may include dislocation or instability, infection, injury to nerves and blood vessels and limb-length discrepancy.
