Total Knee Replacement
Total knee replacement or TKR provides effective pain relief and function improvement in most patients.
In particular, you may benefit from TKR if you suffer from:
- Severe osteoarthritis.
- Rheumatoid arthritis.
- Arthritis secondary to severe gout, pseudogout, and bleeding disorders.
- Osteonecrosis (avascular necrosis – death of bone tissue due to low blood supply).
Dr Sunil Reddy specialises in total knee replacement (TKR) surgery. He utilises the most up-to-date and evidence based technologies to deliver best possible outcomes for his patients. Patient-specific technology (also called PSI-TKR) or Custom knee replacement surgery) and Computer-assisted surgery ( CAS-TKR) , also called Computer-navigated TKR are routinely used in his practice to optimise accuracy and precision.
Dr Reddy also has special interest in Enhanced Recovery Pathways ( ERAS) in knee and hip replacement surgery. The Joint Replacement Clinic has developed pain management protocols and blood-loss minimisation protocols that are routinely implemented in patients to enable day-of-surgery mobilisation, minimise post-operative pain and swelling and enhanced recovery and rehabilitation.
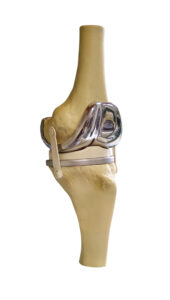
A model of a Total Knee Replacement

The procedure involves replacing the knee joint with a prosthesis (an artificial joint), and in Dr Reddy’s practice takes about 60-70 minutes.
It’s performed under a general anaesthetic or a spinal/epidural anaesthetic. Femoral nerve block may be used as a part of multi-modal peri-operative pain management.
The surgery is performed through an incision in front of the knee joint. Following exposure of the joint, careful and accurate cuts of the distal femur (thigh bone) and proximal tibia (shin bone) are performed to seat the prosthetic components.New technologies in Total Knee Replacement (TKR) are continuously evolving to improve patient outcomes, reduce recovery times, and enhance the precision of surgical procedures.
Specific technologies that Dr Reddy routinely utilises in his TKR practice are explained below. Best patient outcomes are achieved by marrying the latest technologies to innovations in enhanced bio-materials, advanced imaging, pain management modalities and most importantly a holistic patient-centred care model. This has been the objective and ethos of The Joint Replacement Clinic.
Helpful videos
Total Knee Replacement
Total Knee Replacement (Computer-Assisted Robotic Knee Replacement)
Learn more about TKR
Patient-specific technology in TKR
Patient-specific Total knee replacement is a technology that uses MRI scan or CT scan to create 3D models of your knee and then make custom-designed cutting blocks. It is also called Customised Total Knee replacement. It enhances precision and personalisation of TKR surgery.
Patient-specific TKR has two facets:
- Custom Surgical Guides: PSI uses preoperative imaging (CT or MRI scans) to create custom guides tailored to the patient’s unique anatomy. These guides assist the surgeon in accurately cutting the bone and placing the implant, leading to better alignment and fit.
- Preoperative Planning Software: Advanced software allows for detailed preoperative planning. Surgeons can simulate the surgery, optimize implant size and positioning, and foresee potential challenges before entering the operating room.
Advantages of Patient-specific TKR include:
- PSI enables the surgeon to preoperatively better appreciate bone defects and deformities in severe osteoarthritis
- The procedure begins before the surgery. Pre-operatively bone cuts, implant position, implant size, and need for augments is planned on the 3D models from MRI or CT scans.
- Improved accuracy and precision of bone cuts
- Theoretically allows for less-invasive surgery, decreased blood loss and improved post-operative pain.
- It is advantageous in patients with post-traumatic limb deformities or nails and plates from previous fractures.
Robotic-assisted TKR
The use of robotic technology in total knee replacement (TKR), particularly robotic-assisted total knee arthroplasty (r-TKA), is an evolving area that focuses on improving surgical precision and patient outcomes. The evidence suggests that robotic systems may enhance the accuracy of implant positioning, which is crucial for the alignment and longevity of the knee implant. Studies have shown that robotic-assisted procedures may result in more consistent and precise bone cuts compared to conventional methods (BMJ Open).
However, the evidence supporting the widespread adoption of robotic TKR is not yet definitive. The clinical and cost-effectiveness of robotic TKR are still under investigation. Some studies have suggested potential benefits in terms of reduced hospital stays, lower rates of postoperative complications and improved early functional recovery (BMJ Open). Nonetheless, these findings are not supported by larger, randomized controlled trials to establish more robust conclusions, especially regarding long-term outcomes and overall health economics.
Furthermore, while robotic systems provide advanced technological features like real-time data and feedback during surgery, the transition from traditional methods involves a learning curve and significant additional costs related to the robotic equipment. Surgeons are also limited by the choice of implants as most robotic systems are industry-driven and implant-specific. The impact of these factors on the overall adoption and effectiveness of robotic systems in clinical practice remains a subject of ongoing research (BioMed Central). As this field continues to develop, more high-quality studies are required to validate the benefits and understand the limitations of robotic-assisted TKR.
You and your TKR – things you need to know
Overview of benefits
TKR surgeries are incredibly advanced and time-tested treatments that significantly improve your quality of life and let you pursue activities and hobbies you loved to do.
Nine out of ten patients are generally happy with the results of TKR surgery.
Overview of risks
Risks include but are not limited to:
- Injury to blood vessels and nerves (rare complication).
- Infection (less than 1 in 100 surgeries on average).
- Blood clots in the leg veins or lungs (deep venous thrombosis, pulmonary embolism).
- Stiffness of the knee following surgery.
- Wound healing issues.
- Anaesthetic complications.
Although the artificial joint may well last a lifetime, it can also wear out or come loose so a revision knee replacement surgery could be required.
In symptomatic advanced knee arthritis, the benefits of the procedure far outweigh the risks associated.
Dr Sunil Reddy will discuss with you the benefits, risks, and complications at your initial consultation and help you make the best treatment choice.
Enhanced Recovery After Surgery ( ERAS)
Dr Reddy provides Enhanced Recovery After Surgery ( ERAS) pathways to all his knee, hip and shoulder replacement patients. ERAS protocols for total knee replacement (TKR) incorporate a comprehensive, multidisciplinary approach to the perioperative care of patients, aiming to expedite recovery and improve outcomes. This is achieved through a combination of measures including but not limited to pre-habilitation, optimal anaesthetic techniques, LIA (Local Infiltrative Anaesthesia), surgery without tourniquet, blood loss minimisation medication (Tranexamic acid) and less invasive surgical technique.
Hospital stay
Most patients go home within two to three days after a knee replacement. This is in part made possible by ERAS protocols followed at the Joint Replacement Clinic.
Some patients need an overnight observation in HDU (high dependency unit) or ICU (intensive care unit).
Dr Reddy and the Physiotherapist will see you on the same evening or next morning and get you up and about and doing exercises / walking as you can tolerate.
You can go home when you can walk around and feel confident and comfortable to take care of yourself at home, often with assistance from family or friends.
Pain relief and blood loss minimisation
Pain relief during and after your surgery is a priority.
Our anaesthetists are experienced in multi-modality pain relief which includes nerve blocks, IV, oral analgesics, and LIA (local infiltrative analgesia).
Appropriate anaesthesia and IV tranexamic acid in the peri-operative period aid in minimising blood loss and ensure a very low blood transfusion requirement.
Identifying appropriate treatment of anaemia and iron deficiency prior to surgery is an important part of the preoperative evaluation of TKR. If your blood haemoglobin is low, Dr Reddy may advise a period of iron therapy before surgery to give you the best chance of an optimum recovery.
Wound care
Dr Reddy’s Team will see you in the clinic between 12 to 16 days after surgery, unless you live in Country SA when appointment with your GP would be appropriate in this timeframe.
Sutures are absorbable so do not need removal. Please keep the wound clean and dry. The dressing is waterproof enabling you to take a shower.
Please do not remove the dressing before the clinic visit to minimise the risk of infection.
Please do not start antibiotic therapy for perceived wound problems without consulting Dr Reddy.
Call Dr Reddy’s rooms if you have any concerns with excessive pain, redness, or discharge from the wound site, or if you feel unwell.
Rehabilitation guidelines following TKR
The timelines mentioned are approximate and actual progression depends on individual recovery.
Patients can weight bear as tolerated and sit out in a chair on the day of surgery. Please use a walker or crutches until good pain control, quadriceps strength, and walking mechanics are achieved.
Avoid pillows under knees and focus on knee extension and quadriceps exercises from day one. Limb elevation with pillows under ankles / calves when lying is recommended.
Apply ice packs three to five times for 15-20 minutes each time for the first two weeks.
First two weeks
Quadriceps and gluteal sets, proprioception, and balance exercises (e.g. heel-to-toe walking).
- Static and Active Quadriceps exercises
- Straight leg raises as able.
- Active and passive range of movement exercises.
- Gait training.
- Upper body conditioning.
- Please remember to apply ice packs five times daily for 15-20 minutes.
- Take pain medication as advised and follow the advice of your therapist.
Two to six weeks
- Continue with the home exercise program.
- Progress to walking outside.
- Progress with quadriceps, range of movement, and proprioception / balance exercises.
- Start core-strengthening exercises.
- Hydrotherapy / pool workouts once incisions have healed.
- Aerobic exercises after four weeks as tolerated (e.g. static exercise bike).
Six to 12 weeks
- Add lateral steps and step-ups.
- Single leg stance (eccentric exercises initially).
- Progress with all functional activities including household chores, gardening, and gentle sporting activities.
- Low impact activities only until three months.
- No twisting or pivoting until three months.
- Wean into a home / gym program.
Dr Sunil Reddy has over two decades of experience performing Total Knee replacements, most of them utilising patient-specific or computer-navigation technologies. Below are two of his relevant publications in peer-reviewed medical journals.
- Fickert S, Jawhar A, Sunil P, Scharf HP. Precision of Ci-navigated extension and flexion gap balancing in total knee arthroplasty and analysis of potential predictive variables. Arch Orthop Trauma Surg. 2012 Apr;132(4):565-74. doi: 10.1007/s00402-011-1419-x. Epub 2011 Nov 11.
- Nick Pourgiezis, Sunil P Reddy, Mark Nankivell, Gordon Morrison, John VanEssen, Alignment and component position after patient-matched instrumentation versus conventional total knee arthroplasty. Journal of Orthopaedic Surgery 2016;24(2):170-4.




