Total Hip Replacement
Total hip replacement (THR) is considered one of the most successful treatments in medicine.
95% of patients undergoing THR have a very good outcome with significant pain relief and improvement in function.
THR is an option mainly for people who suffer severe arthritis in the hip. It is also an option for patients suffering from avascular necrosis, which in turn may be caused by many factors including trauma, alcoholism, steroid use, decompression sickness, and more.
The procedure replaces damaged and diseased cartilage and bone from the hip joint with an artificial joint. This is made up of two components: the femoral prosthesis which replaces the ball or femoral head, and the acetabular prosthesis which replaces the socket or acetabulum.
Adelaide orthopaedic surgeon Dr Sunil Reddy performs hip replacements using the most up-to-date and evidence–based technologies and implants. He incorporates multi-modality pain relief protocols and blood loss minimisation measures in all his arthroplasty or Joint Replacement procedures to provide the best possible outcome for you.
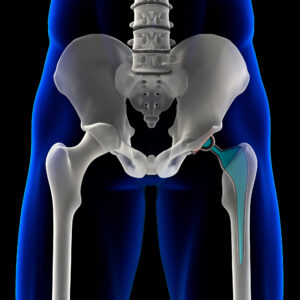
Representative image of THR.
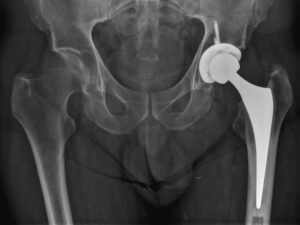
X-ray image of a hybrid THR where bone cement was used for femoral component fixation.

X-ray image of a gentleman with advanced osteoarthritis of both hip joints and after left THR.
Enhanced Recovery After Surgery (ERAS) pathway in Total Hip Replacement
Dr Sunil Reddy and Prof Jegan Krishnan together run The Joint Replacement Clinic. ERAS pathways and protocols for Knee and hip replacement are followed for all patients at JRC.
ERAS protocols for hip replacement surgeries focus on a multidisciplinary, multimodal approach designed to streamline and improve recovery processes. ERAS strategies emphasize reducing minimizing surgical stress, utilisng minimally invasive techniques , decreased length of hospital stay and improving overall patient outcomes. The protocols integrate various stages of patient care, from preoperative education on pain management and expected recovery paths to intraoperative techniques that reduce stress and postoperative practices that promote rapid recovery.
Specific interventions within the ERAS framework for hip replacement that Dr Sunil Reddy routinely employs in his patients include using less invasive surgical techniques, optimising anesthesia, employing multimodal pain management (including local and regional options), and ensuring early postoperative mobilization. Nutritional support, patient education, and the management of preoperative anemia are also crucial elements. The ultimate goals are to reduce complication rates, enhance patient satisfaction, and expedite return to normal function.
Direct anterior approach total hip replacement (DAA-THR)
Dr Reddy performs DAA-THR (sometimes known as anterior minimally invasive total hip replacement) routinely in his patients. Please see the dedicated DAA-THR page on our site to learn more about this procedure.
Dr Reddy has a strong preference for this approach specifically for its advantage in restoring limb lengths accurately, proven decrease in incidence of hip dislocation or instability and for the enhanced recovery pathways it enables. However he also recognises that it is not a suitable approach for every patient with hip osteoarthritis. The decision regarding approach to be utilised is ana individualised one and Dr Reddy will discuss the best options for your specific hip at your consultation. At the end of the day the outcome of your hip replacement surgery depends on sound surgical technique and optimal peri-operative care; and not so much on the approach utilised.
Total hip replacement – things you need to know
Procedure
THR is performed under a spinal anaesthetic or general anaesthesia. A femoral nerve block may be administered for pain relief during and up to 48 hours after surgery.
Dr Reddy as well as your anaesthetist will discuss with you the benefits and risks of the types of anaesthesia and help you decide on the best option for you.
For DAA-THR, with the patient lying supine, an incision about 6-8cm long is used to expose the hip joint using inter-muscular planes. When utilising the Posterior approach, patients lie on the side on the operating table and the hip joint is exposed by detaching and reattaching small tendons and joint capsule on the back of the hip joint. Dr Reddy utilises less-invasive techniques ( eg. SPAIRE approach) when performing posterior approach hip replacement surgery.
The socket as well as the upper end of thigh bone (femur) are then prepared to allow the artificial joint or prosthesis to be inserted.
Dr Reddy uses uncemented implants in most patients younger than 80 years. These implants have a coating on their surface to allow bony integration with the patient’s own socket and femur allowing for a life-long bond. In elderly patients or patients with osteoporosis and poor bone quality, Dr Reddy uses bonecement to bond the femoral prosthesis to bone. This is called a hybrid THR.
When the artificial socket is in place, an artificial lining is inserted. In Dr Reddy’s practice this is made of medical-grade plastic (called UHMWPE or Ultra high molecular weight polyethylene). The new ball may be made of metal or ceramic. Ceramic on poly-ethylene liner bearing has the least amount of wear and suitable for most people undergoing THR.
The procedure normally takes about 60-70 minutes in Dr Reddy’s practice.
Recovery
Dr Reddy will clarify the benefits, risks, and complications of THR at your initial consult. He will give detailed instructions as to how best to recover from surgery. Your therapist will get you to stand and start exercises as tolerated on the day of surgery. Please follow the advice and perform exercises to give yourself the best chance of recovery.
The hospital stay is usually 2-3 days, but this depends on individual recovery. Discharge is criterion-based. You can go home once you feel confident and comfortable walking, transferring to a chair, and managing yourself at home with the help of a friend or family. Sometimes, transfer to a rehabilitation facility is required before you gain the strength and confidence to go home, especially in the elderly and people living by themselves at home.
Avoid sitting on very low chairs and toilet seats and take precaution when getting in or out of a car, especially for the first three months. This is to decrease the risk of dislocation.
Your hip replacement is stable and strong enough to take loads allowing full weight bearing, walking, and activities without restrictions from day one. Normal (i.e. not sport or heavy physical) activity can generally be resumed within three to four weeks of surgery.
Patients can resume or take up some sports after a THR. Sports such as golf, bowls, walking, ‘gentle’ skiing, and doubles tennis are for example perfectly possible. Any sport involving running or contact is not recommended.
THR is not as physiotherapy intensive as a total knee replacement. Walking regularly and performing exercises as detailed below at home is all that is required in most patients.
Overview of risks
- Infection (about 1 in 150).
- Nerve injury resulting in numbness and weakness of leg.
- Blood clots (deep vein thrombosis and pulmonary embolism).
- Limb length discrepancy.
- Fracture of the femur during or after surgery.
- Early loosening of the implants can occur due to failure of bonding with bone or late loosening can occur due to polyethylene wear and osteolysis.

