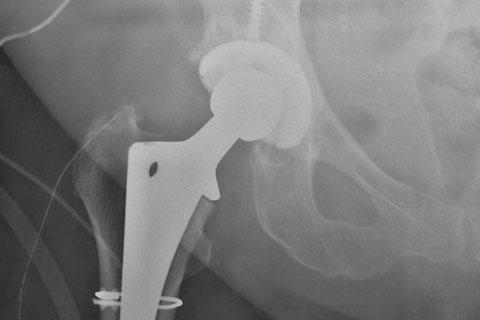
Hip arthroplasty, or the hip replacement procedure, is regarded by many medical experts as one of the most significant advances in medical science of the past fifty years. The vast majority of the millions of patients worldwide undergoing the procedure have as a result enjoyed a vastly improved quality of life, and a 2018 study in Clinical Orthopaedics and Related Research in fact showed a slight increase in longevity over the general population for the 10 year period after surgery.
However, there can still be complications after the procedure, one of which is 'Prosthetic Joint Infection' (PJI) which, although very uncommon (affecting less than 1% of patients) is a serious complication that invariably requires revision surgery.
The main risk factors for PJI are relatively well understood. These are immune deficiencies (eg lymphoma, HIV) and treatments that suppress the immune system (eg chemotherapy, corticosteroids), diabetes, peripheral vascular disease, and obesity.
Two recent studies have shed more light on risk factors for PJI and the effectiveness of revision surgery options.
The first is a very recent study* conducted in the UK into PJI (Prosthetic Joint Infection), which examined longer term outcomes from hip replacement surgery in a cohort of over 600,000 procedures conducted in England & Wales between 2003 and 2013.
In the study, the authors were interested in the risk of revision surgery as against general risk factors, and divided results into elapsed time periods after surgery, in five different time periods from 0-3 months to 24 months and over.
The results identified a number of general factors linked to increase risk of PJI. These were...
- Men more affected than women
- Smoking
- Increasing BMI
- Steroid use
- Previous joint surgery
- Diabetes
- Rheumatoid arthritis
- Depression
There were also some - perhaps counterintuitive - findings, such as that, during the first 6 months after the procedure, patients over 70 were at lower risk of PJI than patients aged under 60. Another finding was that the posterior surgical approach had the lowest risk of revision due to PJI than other methods. The type of prothesis also impacted the risk of PJI, with metal-on-metal types at higher risk than other types (eg ceramic-on-ceramic and ceramic-on-polyethylene) after the initial 24 month period.
In addition to the commonly identified risk factors (above), CPD, dementia, liver disease and congestive heart failure were also correlated with increased risk of PJI in the study.
The second study** was conducted at the University of Bristol in April this year, and focused on revision procedures, and whether there were any differences in incidence of PJI between single stage and two-stage revision procedures.
The single stage approach involves the removal of the affected prosthesis and any affected tissue and the insertion of a new joint during the same procedure. The two-stage approach involves the affected prosthesis being removed in one operation and the patient then being treated for several months with antibiotics before a second procedure to fit the new prosthesis.
The study involved the review of 44 previous studies and found that a single stage procedure was at least as effective if not more effective than the two-stage approach, which is counter to current thinking. The lead researcher, Dr Setor Kunutsor, suggested that further research be conducted to check the initial findings of the research.
*Risk factors associated with revision for prosthetic joint infection after hip replacement: a prospective observational cohort study 25 July 2018
**One- and two-stage surgical revision of peri-prosthetic joint infection of the hip: a pooled individual participant data analysis of 44 cohort studies






